All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the MPN Advocates Network.
The MPN Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the MPN Hub cannot guarantee the accuracy of translated content. The MPN Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The MPN Hub is an independent medical education platform, sponsored by AOP Health, GSK, and Novartis, and supported through educational grants from Blueprint Medicines, Incyte, and Bristol Myers Squibb. The funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View MPN content recommended for you
Diagnostic performance of EPO and JAK2 mutation
A diagnosis of polycythemia vera (PV) is made following various assessments including hemoglobin (Hb) and hematocrit (HCT) levels, red cell mass (RCM) isotopic measurement, bone marrow biopsy histology, JAK2 mutation, serum erythropoietin (EPO) level, and endogenous erythroid colony (EEC) formation. JAK2 mutation is classed as a major criterion for myeloproliferative neoplasms (MPN) and is a first-line test if there is acquired erythrocytosis present. EEC was classed as a major criterion, but was gradually downgraded, possibly due to it being a difficult to standardize laborious technique to measure. Serum EPO is a minor criterion in adults yet is included in key decision trees in children. Maslah et al.1 recently assessed the diagnostic performance of EPO and JAK2 mutations in well characterized patients with RCM measurements suspected to have PV, and published their findings in the British Journal of Haematology, summarized below.
Study design and patient characteristics
This cohort study included 1,090 patients, who attended Hôpital Saint-Louis, Paris, FR, between 2010 and 2018 in whom RCM, EPO, and JAK2 status was known. Patients were predominantly male and had a median age of 59.4 years (Table 1). True PV was defined as an RCM of ≥125% of the theoretical normal value, considering age, sex, and weight. Serum EPO values of 3.3–16.6 mUI/mL were considered normal. Patients were referred for RCM and plasma volume tests following elevated HCT and/or Hb, and/or a high platelet count, which may be indicative of PV or MPN.
Table 1. Patient characteristics*
|
EPO, erythropoietin; Hb, hemoglobin; HCT, hematocrit; RCM, red cell mass. |
|
|
Characteristic |
Value/patients |
|---|---|
|
Median age, years (range) |
59.4 (13.6–92.7) |
|
Median Hb, g/dL (range) |
17.2 (11.5–21.4) |
|
Median HCT, % (range) |
49.8 (34.9–66.1) |
|
Median leucocytes, G/L (range) |
7.5 (2.3–90) |
|
Median platelets, G/L (range) |
234 (60–2,077) |
|
High HCT/Hb†, % |
70.1 |
|
Median RCM, % of theoretical value (range) |
131 (67–259) |
|
RCM ≥125%, % |
72.1 |
|
High HCT/Hb† and an increased RCM (≥125%), % |
56.0 |
|
JAK2 mutation present (V617F or exon 12), % |
28.3 |
|
EPO |
|
|
Median, mUI/mL (range) |
6.5 (<0.6–969) |
|
Very low (≤1.99 mUI/mL), % |
9.9 |
|
Low (≤3.30 mUI/mL), % |
25.0 |
|
Normal (3.30–16.60 mUI/mL), % |
67.0 |
|
High (≥16.60 mUI/mL), % |
8.0 |
Results
Of the patients included in the study, 70.1% had high HCT and/or Hb levels (based on World Health Organization [WHO] criteria; Table 2), with 80% of those being diagnosed with true PV. Of the patients who had normal HCT and/or Hb levels (29.9%), 54% were diagnosed as true PV (Figure 1). Interestingly, all male patients with an HCT ≥57.9% or Hb ≥19.8 g/dl, and all female patients with an HCT ≥57.6% or Hb ≥18.3 g/dl had true PV, demonstrating that RCM measurements were not necessary for true PV diagnosis in these patients. In patients who had a high HCT/Hb level, the presence of low EPO levels could predict true PV with a 92% positive predictive value (PPV), and a JAK2 mutation with a 90% PPV. By combining the two measurements, PPV increased to 94%, meaning that if RCM measurements are not possible, these measurements will enable diagnosis of true PV to be made with a 6% risk of it being a false positive. The exact cutoff point for low EPO levels affected the sensitivity of diagnosis, varying from 91.2% for EPO ≤3.30 mUI/mL, to 73.7% for EPO ≤1.99 mUI/mL. The lower threshold yielded a specificity and PPV of 100%.
Figure 1. Diagnostic charts of suspected PV patients*
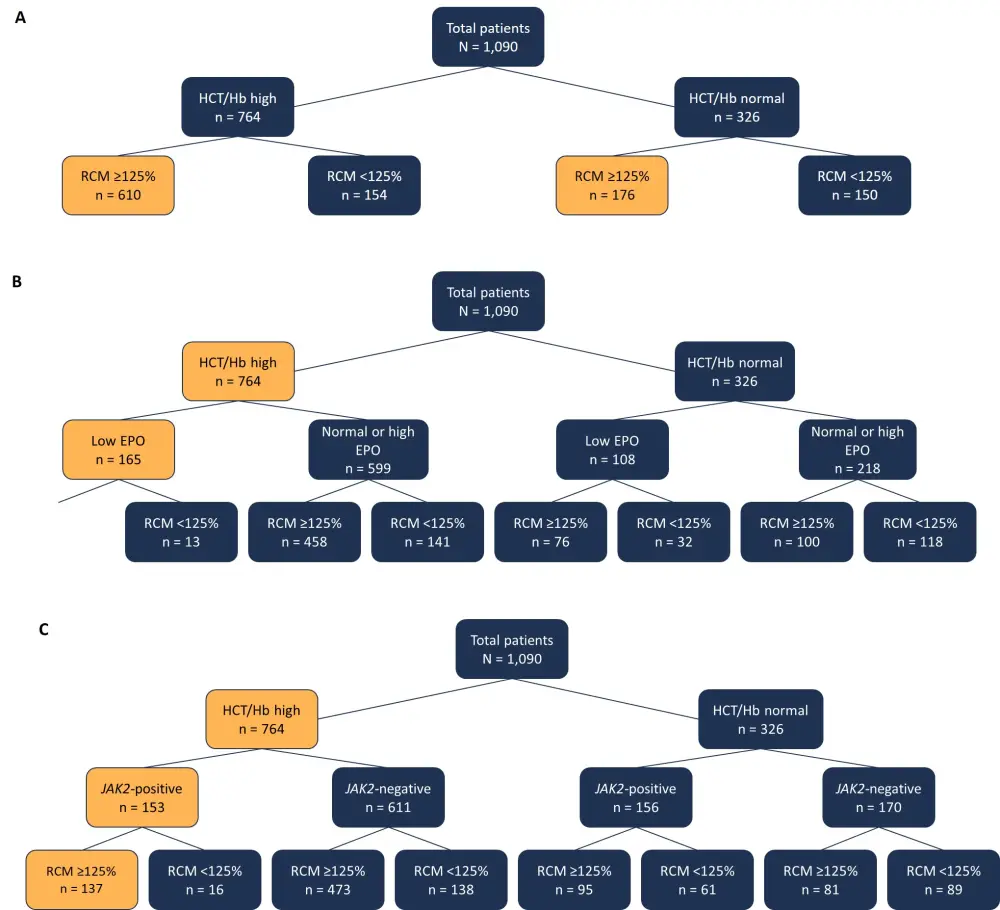
(A) Proportion of patients with true PV (RCM ≥125%) in patients with either a high HCT/Hb or normal HCT/HB. (B) Proportion of patients with true PV (RCM ≥125%) if EPO is the first test performed. (C) Proportion of patients with true PV (RCM ≥125%) if JAK2 mutation is the first test performed.
EPO, erythropoietic; Hb, hemoglobin; HCT, hematocrit; PV, polycythemia vera; RCM, red cell mass.
*Adapted from Maslah et al.1
Although there were 125 patients with a low EPO and a JAK2 mutation in the high HCT/Hb and high RCM group, and 66 in the normal HCT/Hb, high RCM group, Maslah et al.1 felt that assessing both was unnecessary in true PV patients. There were 37 cases with a low EPO and no JAK2 mutation (discrepant cases) in these groups that may be explained by a rare JAK2 mutation or a mutation in the EPO receptor. No further assessments were made in these patients as the WHO 2016 criteria were not met, suggesting a limitation in diagnosing PV in these cases.
There was a second group of discrepant cases (n = 41) who have a normal or high EPO level, but also a JAK2 mutation. In 20 of these patients, this could be explained by secondary erythrocytosis due to pulmonary or cardiac insufficiency, sleep apnea, arrhythmia, smoking, and obesity. The team observed an inverse correlation between EPO level and RCM in PV patients (RCM ≥125%, high HCT/Hb and presence of a JAK2 mutation), but in JAK2 wild-type patients (RCM ≥125% and high HCT/Hb), they noted a positive correlation between EPO level and RCM. Lastly, the study highlighted a correlation between JAK2V617F allele burden and RCM. In patients with JAK2 mutation, RCM was higher compared with JAK2 wild-type patients regardless of the HCT level, and this difference between two groups increased with HCT level.
Conclusion
Maslah et al.1 demonstrated that a high HCT/Hb level and a lower-than-normal EPO level, was as efficient at diagnosing true PV. They could not rule out possible bias at recruitment, as RCM is not performed in all patients with PV. However, they highlight the large patient sample, and homogeneous criteria, and well standardized tests used for the assessment as advantages of the study, and conclude that EPO should be revisited as a major criterion for diagnosis.
Additional content
In 2017, updated PV diagnostic criteria were published by the WHO in their 2016 classification system for tumors of the hematopoietic and lymphoid tissues. Table 2 details the diagnostic criteria for adults: all three major criteria, or the first two and one minor criterion, must be met for PV diagnosis.
Table 2. 2016 WHO diagnostic criteria for adult PV*
|
BM, bone marrow; Hb, hemoglobin; HCT, hematocrit; PV, polycythemia vera; RCM, red cell mass; WHO, World Health Organization. |
|
|
Major criteria |
|
|
1 |
Hb >16.5 g/L in men, >16.0 g/L in women |
|
2 |
BM biopsy with hypercellularity for age with trilineage growth, and megakaryocytic proliferation with pleomorphic, mature megakaryocytes |
|
3 |
Presence of JAK2V617F or JAK2 exon 12 mutation |
|
Minor criteria |
|
|
1 |
Subnormal erythropoietin level |
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

