All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the MPN Advocates Network.
The MPN Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the MPN Hub cannot guarantee the accuracy of translated content. The MPN Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The MPN Hub is an independent medical education platform, sponsored by AOP Health, GSK, and Novartis, and supported through educational grants from Blueprint Medicines, Incyte, and Bristol Myers Squibb. The funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View MPN content recommended for you
COMFORT-I and -II trials: Post hoc analysis
Currently, ruxolitinib is used for the treatment of patients diagnosed with intermediate- or high-risk myelofibrosis.1 Results from the phase III COMFORT trials have shown ruxolitinib to reduce spleen volume, improve disease-related symptoms, and prolong overall survival. The COMFORT-I trial compared ruxolitinib therapy with placebo and the COMFORT-II trial compared ruxolitinib with best available treatment.1
During the European Hematology Association (EHA) 2023 Congress, post hoc analysis results investigating the impact of new or worsening anemia on spleen volume response and total symptom score (TSS) in patients diagnosed with myelofibrosis and treated with ruxolitinib were published.1 We summarize the key findings below.
Stud design
- Patients were administered ruxolitinib twice daily.
- 15 mg for patients with a platelet count of 100–200 × 109/L
- 20 mg for patients with a platelet count >200 × 109/L
- The primary endpoints were:
- The proportion of patients with a reduction in spleen volume of ≥35% from baseline (SVR35) at Week 24 and Week 48
- Patients with a ≥50% reduction in TSS at Week 24
Results
- A total of 277 patients were included in the analysis.
- 55.6% of patients at baseline were nonanemic.
- 19.9% of patients at baseline were anemic but not transfusion dependent.
- 24.5% of patients at baseline were anemic and transfusion dependent.
- The percentage of patients achieving SVR35 with new or worsening anemia up to Week 12 according to anemia status and transfusion dependence were similar (Figure 1).
Figure 1. Percentage of patients achieving SVR35 with new or worsening anemia according to anemia status and transfusion dependence*
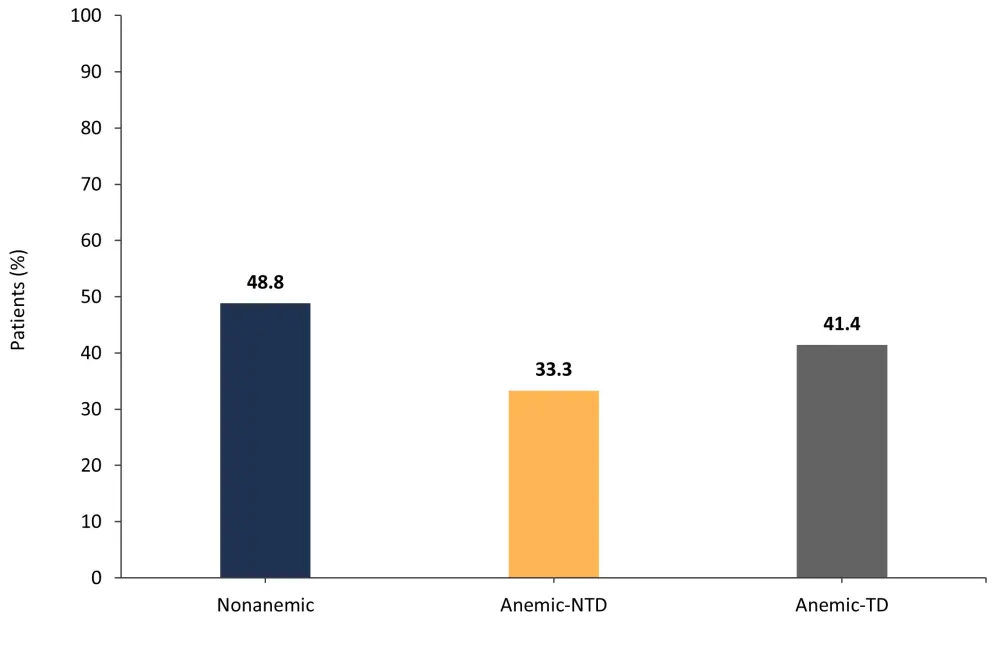
NTD, non-transfusion dependent; TD, transfusion dependent; SVR35, spleen volume reduction of ≥35%.
*Adapted from Mauro.1
- In contrast, a higher percentage of patients who were nonanemic and showed no new or worse anemia up to Week 24 achieved SVR35 compared with patients who were anemic and were either non-transfusion or transfusion dependent (Figure 2).
Figure 2. Percentage of patients achieving SVR35 with no new or worsening anemia according to anemia status and transfusion dependence*
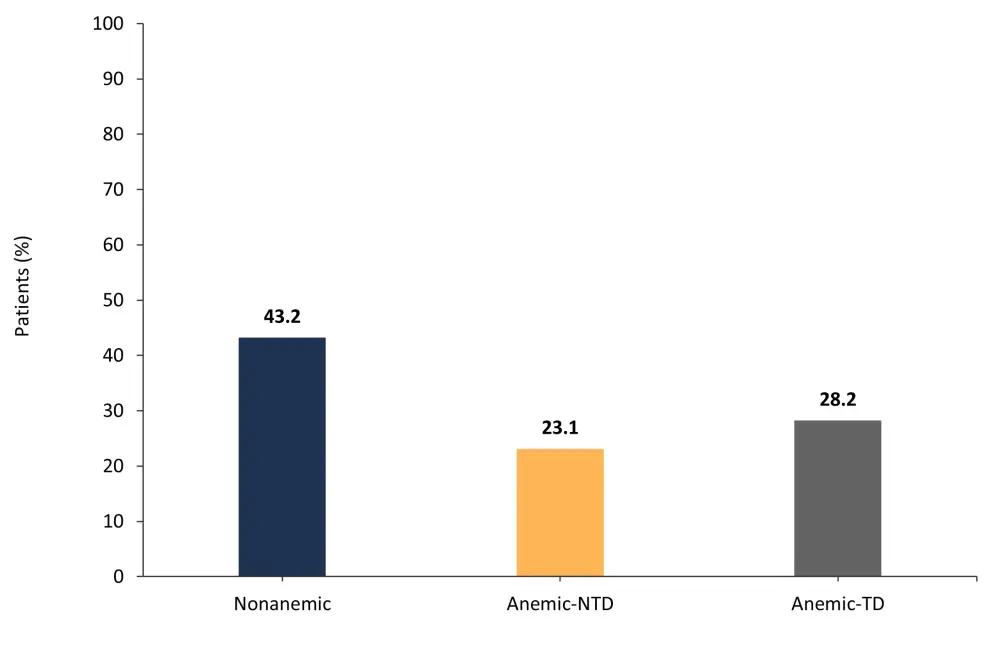
NTD, non-transfusion dependent; TD, transfusion dependent.
*Adapted from Mauro.1
- The percentage of patients achieving SVR35 at Week 48 were similar regardless of anemia and transfusion dependence status.
- The proportions of patients with new or worsening anemia up to Week 12 and ≥50% reduction in TSS at Week 24 were:
- Nonanemic, 51.1%
- Anemic and non-transfusion dependent, 42.1%
- Anemic and transfusion dependent, 46.7%
- The proportions of patients with no new or worsening anemia up to Week 12 and ≥50% reduction in TSS at Week 24 were:
- Nonanemic, 42.9%
- Anemic and non-transfusion dependent, 40.0%
- Anemic and transfusion dependent, 54.2%
Conclusion
Patients treated with ruxolitinib experienced decreased spleen volume and improved TSS regardless of anemia and transfusion dependence status. Furthermore, new or worsening anemia after baseline had no effect on the efficacy of ruxolitinib compared with patients who experienced no new or worsening anemia.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

