All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the MPN Advocates Network.
The MPN Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the MPN Hub cannot guarantee the accuracy of translated content. The MPN Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The MPN Hub is an independent medical education platform, sponsored by AOP Health, GSK, and Novartis, and supported through educational grants from Blueprint Medicines, Incyte, and Bristol Myers Squibb. The funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View MPN content recommended for you
ET in adults ≥60 years: A multicenter real-world study in China
Essential thrombocythemia (ET) is a subtype of BCR::ABL1-negative myeloproliferative neoplasms (MPN), and approximately 50% of patients who are diagnosed with ET are ≥60 years old.1 The MPN Hub have previously reported on a study investigating key considerations in diagnosing and treating pediatric patients with MPN, with specific mention of ET. Below, the MPN Hub describes a retrospective analysis evaluating older patients (≥60 years) and the potential need for different treatment strategies and prognosis compared with younger patients (18-59).
Study design1
This retrospective, real-world analysis compared the differences in the molecular characteristics, risk factors for complications and disease progression, and current treatment status of patients diagnosed with ET from China.1 Eligible patients:
- Were aged ≥60 years or between 18–59 years (control group)
- Had a diagnosis of ET according to the World Health Organization 2016 criteria2
- Had no previous diagnosis of polycythemia vera, primary myelofibrosis (MF) or prefibrotic primary MF.
Selected baseline characteristics of older patients with ET are shown in Table 1.
Table 1. Baseline characteristics*
|
L, liter; WBC, white blood count. *Adapted from Fu, et al.1 |
||
|
Characteristics, % (unless otherwise specified) |
Hydroxyurea treatment (n = 160) |
Interferon α treatment (n = 31) |
|---|---|---|
|
Sex |
||
|
Female |
51.3 |
38.7 |
|
Male |
48.8 |
61.3 |
|
Median age (range), years |
67 (60–91) |
65 (60–77) |
|
Median WBC (range), x109/L |
10.3 (4.5–27.1) |
11.34 (5.24–25.7) |
|
Driver mutations |
||
|
JAK2V617F |
67.5 |
64.5 |
|
CALR |
14.4 |
9.7 |
|
MPL |
2.5 |
6.5 |
Results1
A total of 903 patients were included in the analysis, of which 282 patients were aged ≥60 years and 621 patients were aged between 18-59 years acting as the control population. Older patients (≥60 years):
- Had a significantly different genetic mutation profile compared with the control group (Figure 1).
- Had higher white blood count, neutrophil count and platelet counts compared with the control group.
- Had higher rates of thrombosis before diagnosis (37.23% vs 13.69%) and during follow-up (20.21% vs 4.83%).
- At follow-up, 8.16% of patients had disease progression to MF (2.13% vs 1.61%, p = 0.592) or acute leukemia (6.03% vs 5.48%, p = 0.739) compared with the control group.
Figure 1. Genetic mutation profile of patients aged ≥60 years compared with control group*
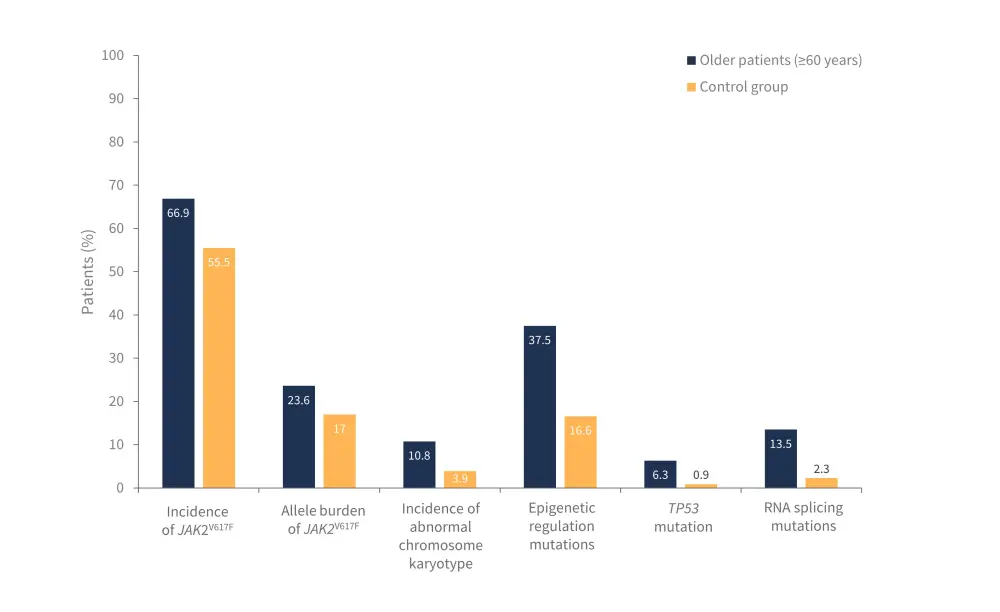
RNA, ribonucleic acid.
*Adapted from Fu R, et al.1
Safety
Among the patients aged ≥60:
- Risk factors for disease progression were presence of palpable splenomegaly, male sex, and presence of ASXL1 and SF3B1 mutations.
- Overall, 34 patients died after a median duration of 45.45 months from diagnosis.
- Of these patients, 15 died from ET, five from thrombotic complications, one from cerebral hemorrhage, and nine from disease progression.
- More patients died from ET (5.32% vs 1.45%), thrombotic events (1.77% vs 0.16%) and disease progression (3.19% vs 1.13%) compared to the control group.
Real-world treatment status in older patients (≥60 years)1
According to the National Comprehensive Cancer Network, all patients who are at high-risk for ET should receive cytoreductive therapy combined with antiplatelet drugs.
- In real-world setting, 57.08% of patients were categorized as high-risk and were in line with these guidelines.
- Meanwhile, 50.55% of older patients with ET evaluated in this study were categorized as high-risk and were in line with these guidelines.
Conclusion
This study suggests that patients diagnosed with ET who were aged ≥60 years have different clinical characteristics, molecular profiles, thrombotic and bleeding complications, and prognoses compared with patients aged 18-59 years. These findings indicate that older patients may benefit from different treatment regimens than younger patients and highlights the need for further studies and reviews of clinical practice in this population.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content


